Have you recently been diagnosed with Chronic Kidney Disease (CKD)? If so, you may be feeling overwhelmed, unsure which information to trust, or confused by medical terms. Suddenly you’re hearing acronyms like CKD, and lab values such as creatinine and GFR discussed at appointments — and you may be wondering where to even begin with nutrition.
You’re not alone. Here are five important things to know as you get started.
1. You’re Not Alone — and Nutrition Matters
An estimated 37 million adults in the United States are living with CKD, and about 1 in 3 adults are at risk due to conditions like diabetes, high blood pressure, or family history. Because early CKD often has no symptoms, roughly 90% of people don’t realize they have it.
The good news: early nutrition changes can make a meaningful difference.
If your doctor has recently mentioned CKD — or you’ve noticed abnormal lab values such as: creatinine, BUN (blood urea nitrogen), potassium, and phosphorus — it’s a great time to connect with a kidney dietitian. Research has shown that nutrition is a powerful tool for CKD management, but this is not a do-it-yourself journey! The internet can be overwhelming with conflicting information when it comes to kidney nutrition advice. A specialized dietitian can guide you from confusion to clarity, helping you make confident, personalized decisions.
Understand CKD Stages
Learning the basics of CKD staging can help you better understand your health and treatment goals. This short video provides a helpful overview of how CKD is diagnosed and staged: https://youtu.be/OSNXwuvP910
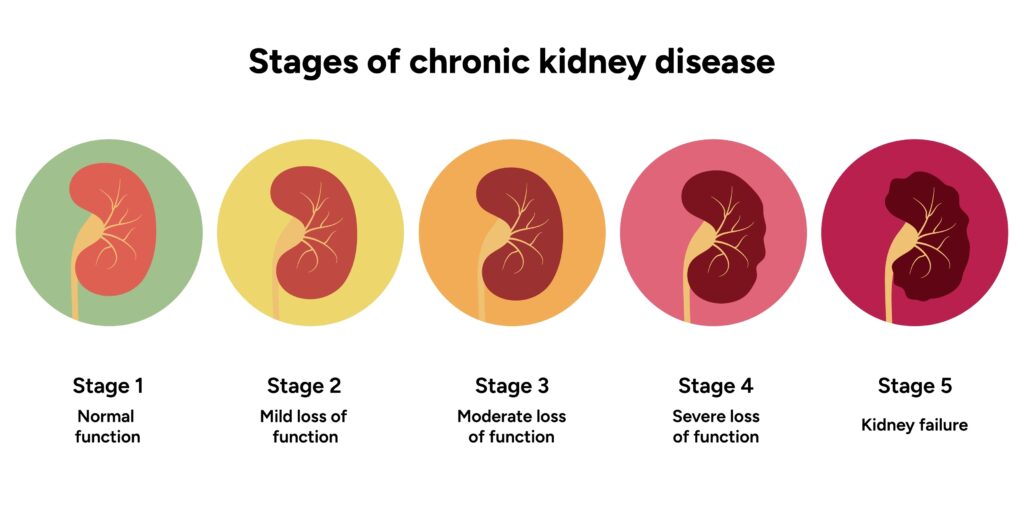
Nutritional priorities shift depending on your stage of CKD, and recommendations should always be individualized. While many healthcare professionals provide valuable guidance, kidney dietitians have expertise in managing nutrition across all stages of kidney disease and can help tailor recommendations to your needs.
2. Protein: Finding the “Just Right” Balance
Recent research (1) showed that appropriate protein intake in CKD led to:
✅ 41% lower risk of kidney failure (OR 0.59)
✅ Reduced risk of end-stage kidney disease (OR 0.64)
✅ Slower decline in eGFR
✅ Lower proteinuria and phosphorus levels
With that being said, protein intake requires careful balance in CKD. Too much protein may place extra strain on the kidneys, while too little can weaken the body, increase inflammation, and affect overall health.
Think of it as the Goldilocks principle — not too much, not too little, but just right.
Common protein sources include meat, fish, eggs, dairy, beans, soy, nuts, and seeds. Many people find that incorporating plant-based meals can be gentler on the kidneys. A kidney dietitian can help you determine the right amount and sources of protein for your specific situation.
3. Power up with Plants
Eating more plant-based foods (vegetables, fruits, nuts, seeds, and legumes) can reduce kidney workload. Research shows healthy plant-based diets are linked to a 21–26% lower mortality risk (2). Aim for half your plate to be vegetables or a green salad. Start by adding one cup of raw or cooked greens/vegetables to your current diet. Frozen vegetables are equally nutritious; just ensure they have no added sauces or salt. Try different cooking methods like air frying, roasting, and steaming for better results. No one likes mushy veggies!
4. Become a Sodium Sleuth

Sodium plays a major role in blood pressure control, which directly impacts kidney health. The goal isn’t eliminating sodium entirely — it’s finding the right balance. Over-restriction can be harmful, but excess intake can contribute to complications.
Try becoming a “sodium sleuth” by spotting hidden salt in packaged and restaurant foods. Practical targets:
⭐ Low sodium food: ≤140 mg per serving
👍 Good choice: ≤200 mg per serving
⚠️ Limit: >300 mg per serving
🚫 High sodium: ≥400 mg per serving
👉 500–700 mg per meal max
Flavorful low-sodium seasoning options include:
- Magic Chef salt-free seasoning
- Dan-O’s salt-free seasoning
- Mrs. Dash
- Trader Joe’s 21 Seasoning Salute
- MicroSalt
5. Individualization Is Key
Nutrition for CKD is not one-size-fits-all. Dietary needs vary depending on your stage and lab values, including monitoring of:
- Potassium
- Phosphorus
- Protein
- Fluid intake
Your primary care provider or nephrologist tracks these through lab work, while a kidney dietitian translates those results into practical eating strategies tailored just for you.
Key Takeaway
A CKD diagnosis can be scary — no one welcomes this news. But you don’t have to do it alone. Adding a kidney dietitian to your care team can provide practical tips, personalized strategies, and clear explanations that support kidney health and may help slow disease progression.
At Life Cycle Nutrition we have a team of Registered Dietitians that specialize in renal nutrition and have combined experience of over 50 years working with Chronic Kidney Disease! Click here to schedule an appointment today.




0 Comments