Endometriosis and polycystic ovary syndrome (PCOS) were words my OB-GYN uttered years ago after I casually mentioned my common monthly routine of get period, have debilitating cramps, break out into cold sweat, and experience vomiting and diarrhea. Rinse and repeat, month after month. While I ended up not having either condition, I did wonder, what is she talking about?
Definition + Symptoms
Endometriosis is a chronic inflammatory condition that effects an estimated 10% of premenopausal women worldwide. Endometriosis occurs when the same tissue that lines the uterus (and should only be in the uterus) gets a wandering eye and is found elsewhere in the body, including the ovaries, fallopian tubes, bladder, C-section scars, and bowel.
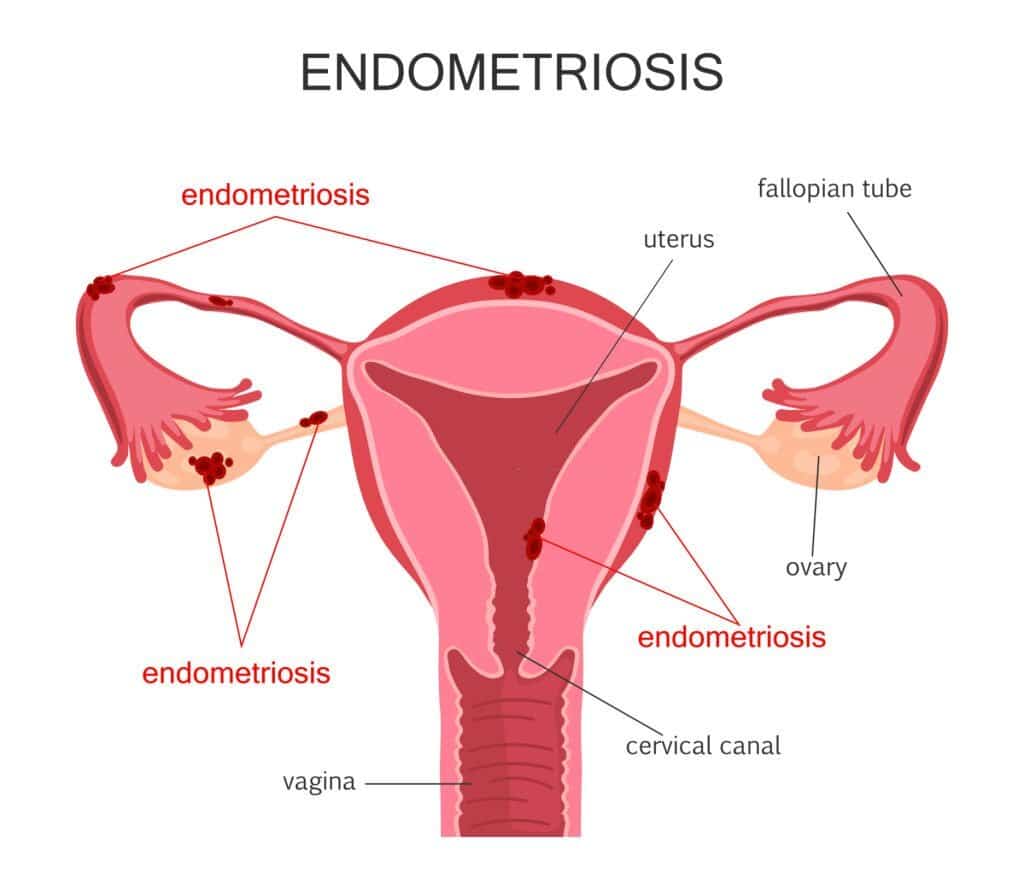
Just as the uterine lining builds and sheds each month in response to our hormones, so does the same endometrial tissue found outside the uterus. The only problem is that it can’t leave the body through the vagina, so it sheds into the pelvic cavity, forming scar tissue that causes chronic inflammation, an immune response, and worsening symptoms.
Depending on where the lesions are located, women may experience intense pelvic pain, severe cramping, heavy menstrual flow, pelvic floor dysfunction, IBS symptoms, nausea, depression, anxiety, painful sex, and infertility.
Causes + Diagnosis
The jury is still out on what causes endometriosis; however, researchers have found that it has almost all the indications of an autoimmune condition, and is found to occur in conjunction with other autoimmune conditions such as Hashimoto’s thyroiditis, Celiac disease, multiple sclerosis, and inflammatory bowel diseases.

Some researchers have attributed this immune and inflammatory response to gut health, particularly lipopolysaccharides toxins (LPS) and small intestinal bacterial overgrowth (SIBO). Other possible contributing factors in the development of endometriosis include genetics, lifestyle, and retrograde menstruation (backflow of menstrual blood and uterine tissue into the pelvic cavity).
According to the Mayo Clinic, endometriosis may be diagnosed via ultrasound and MRI. However, the current gold standard is exploratory laparoscopy surgery, which is unfortunately the most invasive choice.

Treatments
While a cure for endometriosis would be fabulous, we’re not there yet, friends. However, there are plenty of things we can do to lessen disease progression, reduce cyst size, relieve symptoms, and place endometriosis into remission.
Heck, even though I wasn’t diagnosed with endometriosis, I still used these lifestyle principles to eliminate my monthly symptoms of debilitating cramps, cold sweats, vomiting, and diarrhea.
- Build a Team. You don’t have to do any of this alone. Hopefully, you already have a great gynecologist or endocrinologist on board that helped with your diagnosis. Next on your list, is to connect with a registered dietitian nutritionist (RDN) who specializes in hormone and gut health, and a physical therapist who specializes in the pelvic floor and visceral work. I’m also a huge advocate for mental health, so if you notice stress, depression, and/or anxiety are interfering with your life, then I’d strongly recommend a mental health practitioner too. And yes, I can provide referrals for all the above.
- Start with the Gut. The majority of our immune system is housed in the gut, so digestive health is the first place to start.
- Mindful Eating. Multiple blog posts could be written about mindful eating alone, so here are some quick tips: savor the smells of your meal, take a few deep breaths or give thanks before eating, chew thoroughly and eat slowly, remove distractions, and enjoy your surroundings (whether it’s people, a nice tablecloth, or mood lighting).
- Up Your Fiber. Fiber is magic for gut health, reducing inflammation, and eliminating toxins and excess hormones like estrogen from the body. Gradually increase fiber at meals or snacks, aiming for ~40 grams of fiber daily from vegetables, fruits, nuts, seeds, legumes, lentils, and whole grains.
- Hydrate Yo’ Self. As you increase fiber, you need to increase water to prevent constipation. A minimum goal for water is half of your body weight in ounces daily. So, if you weigh 150 lbs, then drink 75 oz of water daily (and you may need more based on activity levels, sweating, etc.)
- Go Mediterranean. The Mediterranean diet is well known as an anti-inflammatory diet, which is the bee’s knees for endometriosis. It’s high in omega-3 fatty foods like salmon, sardines, chia seeds, walnuts, and flaxseeds, as well as incorporates a colorful variety of fiber-rich foods as mentioned above. Other therapeutic diets exist that work well for autoimmune-type conditions like endometriosis; however, they can be pretty restrictive, so the Mediterranean diet is a great place to start.
- Supplement. While I’m a “food first” kinda gal, there is great research on specific supplements to support endometriosis. Speak with your RDN or doctor regarding your individual needs for vitamin D, N-acetylcysteine (NAC), magnesium, fish oil, B-vitamins, curcumin, resveratrol, and berberine.
- Address the Stress. While various levels of stress are always going to be a part of our lives, it doesn’t have to rule our lives (trust me, I’m still working on it too). Ways to decrease stress include: prioritizing sleep (get to sleep by ~10 pm to optimize deep sleep), incorporating rest days with exercise days, spending time in a positive community (family, friends, etc.), partaking in activities you enjoy (knitting, reading, robotics, music, etc.), vagus nerve exercises (the “rest and digest” nerve that connects the gut and brain; singing, chanting Om, gargling, etc. help massage it), and utilizing heart rate variability (HRV) to assess stress/inflammation throughout the day and after meals.
- Movement. Studies show that moving your body can also reduce the impact of endometriosis symptoms, such as IBS and PMS, as well at strengthening the pelvic floor.
- Additional Testing. Since endometriosis tends to go hand-in-hand with other autoimmune conditions as well as gut dysbiosis, consider ruling out other autoimmune diseases, and running a breath test for SIBO and the GI Map for gut health.
Small changes create momentum and produce big results. Pick one or two items to work on first. Practice it (progress, not perfection). Every other week or so, add another item from the list and feel your health improve. If you’d like to go more in-depth with these lifestyle principles, I’d love to help! Please email me or schedule an appointment today.
If you thought this blog post was helpful or know someone who would benefit from it, please like it and share it.
With love, Steph



0 Comments